Perhaps it’s growing older, but increasingly I envisage future generations boggling at things I took for granted. The Tube was free all night on New Year’s Eve, I see myself telling envious future grandchildren (it charged standard fares this year). Councils would run massive firework displays with no entrance fee on bonfire night (ours couldn’t afford to last time). We used to know the name of our GP, and call up in the morning for an appointment the next day.
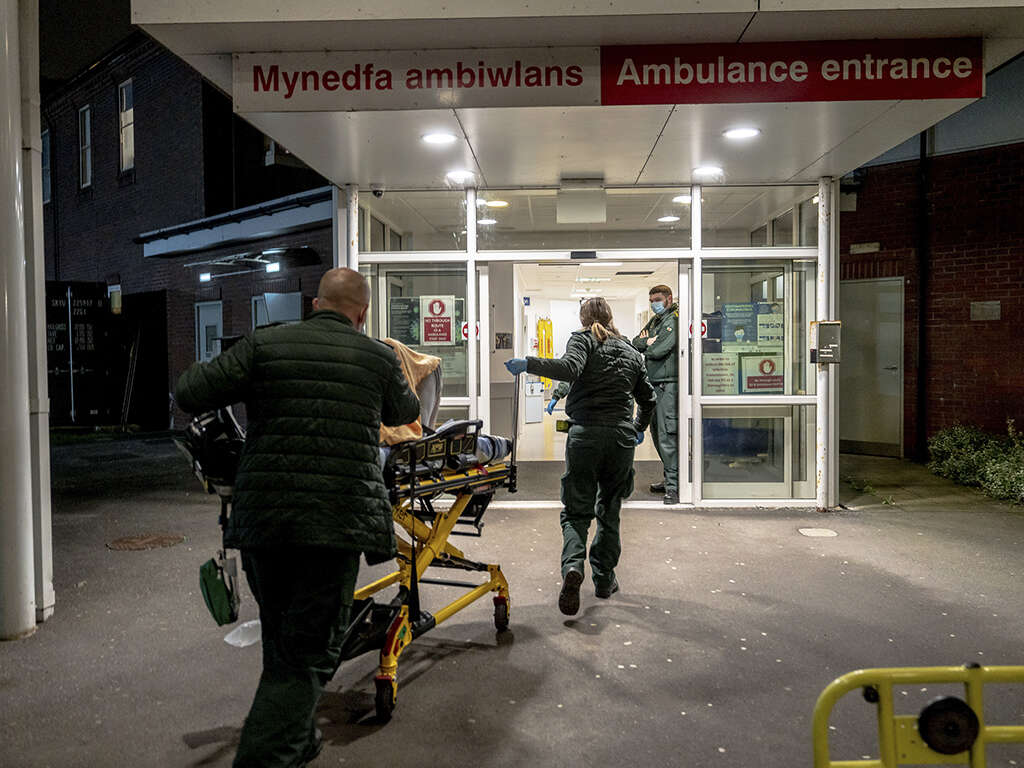
Now, it’s the NHS. Will the idea of an ambulance arriving within minutes also become a memory of an exotic past? Will my grandchildren sigh at my nostalgic ramblings while booking me an Uber999 to hospital? What would that hospital even look like?
This is the true sign of “crisis”. Cataclysmic, transformative, the fallout meaning the landscape may never look the same again. This is what’s happening to the NHS. The term “NHS crisis” had appeared in headlines for so many winters – when more people end up in hospital – that the phrase had become something of a running joke in medical and media circles. It turns out those busy seasons were just warning signs. The build-up to the big one. Now it’s here.
Between 300 and 500 people are dying a week because of emergency response delays, Dr Adrian Boyle, president of the Royal College of Emergency Medicine, warned on New Year’s Day. The number of patients waiting more than 12 hours in A&E to be admitted or discharged has risen 355 per cent compared with last November. There is never a good time to fall ill or have an accident but you definitely don’t want that to happen today.
How has the situation been allowed to get this bad? I’ve spoken to doctors, nurses, paramedics, patients, officials and hospital trust heads about what has been going wrong over the years. The following is a reflection of what they’ve told me.
Let’s start with the obvious: we are barely a year out of a pandemic. Covid-19 added a whole load more patients into the mix in peak flu season. Flu infections, as well as others like strep A and RSV, have been building up after two years of social distancing, masking and enhanced hygiene measures.
At the height of the pandemic people were more reluctant to go into hospital or call the emergency services – the “missing patients” identified by the New Statesman at the time. British citizens were told to “stay at home, protect the NHS, save lives”. Early signs of cancer were missed, conditions worsened, and that pent-up demand is spilling out now. Though controversial, people on the front line I’ve spoken to also tell me patients are now quicker to turn to A&E – sometimes inappropriately – because of dissatisfaction with their GPs or the 111 non-emergency phone service.
[See also: Do the public support the nurses’ strike?]
Health workers endured long, draining shifts throughout the pandemic. Their holidays were repeatedly cancelled at the last minute; some were traumatised by what they saw on Covid wards; it was a physical and mental onslaught. The “catch-up”, working through the backlog that built up during the pandemic, I’m told can be even more stressful than treating Covid itself. Levels of burnout and sickness absences rocketed. By February 2022 NHS staff were quitting at a record rate. Now, more than one in ten nursing jobs in England are vacant.
When asked about the NHS meltdown, ministers love to mention the unique challenges of Covid-19. Yet most of the current mess is the result not of a capricious virus but political decisions. Indeed, it was a political decision in the first place not to keep putting resources into pandemic preparations (the personal protective equipment stockpile was largely out of date when coronavirus hit, for example). The waiting list for procedures, now at a record 7.2 million, was already 4.4 million in February 2020, just before lockdown.
Austerity, when Conservative-led governments began cutting public budgets from 2010, is the backdrop to much of what we’re suffering today. Repeated public sector pay freezes mean NHS jobs are not as well-paid as they were 12 years ago, making them less attractive. Deep cuts to councils have severely stretched social care provision. This is depriving tens of thousands of people taking up hospital beds of care home places or community care packages – an issue at the heart of ambulance handover delays. All while demand is rising, with an ageing population and medical advances lengthening the life spans of disabled people.
Conservative politicians will argue that the NHS’s budget was protected from cuts in this time, and health spending rose. And it did, but at a slower rate than in the preceding decade. The UK spends less on health than its major European counterparts. The number of available overnight hospital beds fell 11 per cent from 2010 to 2020. Outcomes worsened. Every major A&E unit in England failed its four-hour waiting time target for the first time in November 2019.
[See also: How Rishi Sunak is getting away with the NHS crisis]
Brexit made things worse too. Thousands of European doctors decided not to work in the UK because of its departure from the EU. The end of free movement has exacerbated longstanding NHS labour shortages. A more liberal immigration system and better pay and conditions could help, but Rishi Sunak wants to cut net migration to the UK; and he is refusing to negotiate with striking nurses. In November 2021 Tory MPs even voted against publishing the number of staff the NHS needs to recruit, which could have improved workforce planning.
So if you are unlucky enough to have an emergency this winter, remember the carnage around you was a political choice. And remember how it used to be.







Join the debate
Subscribe here to comment