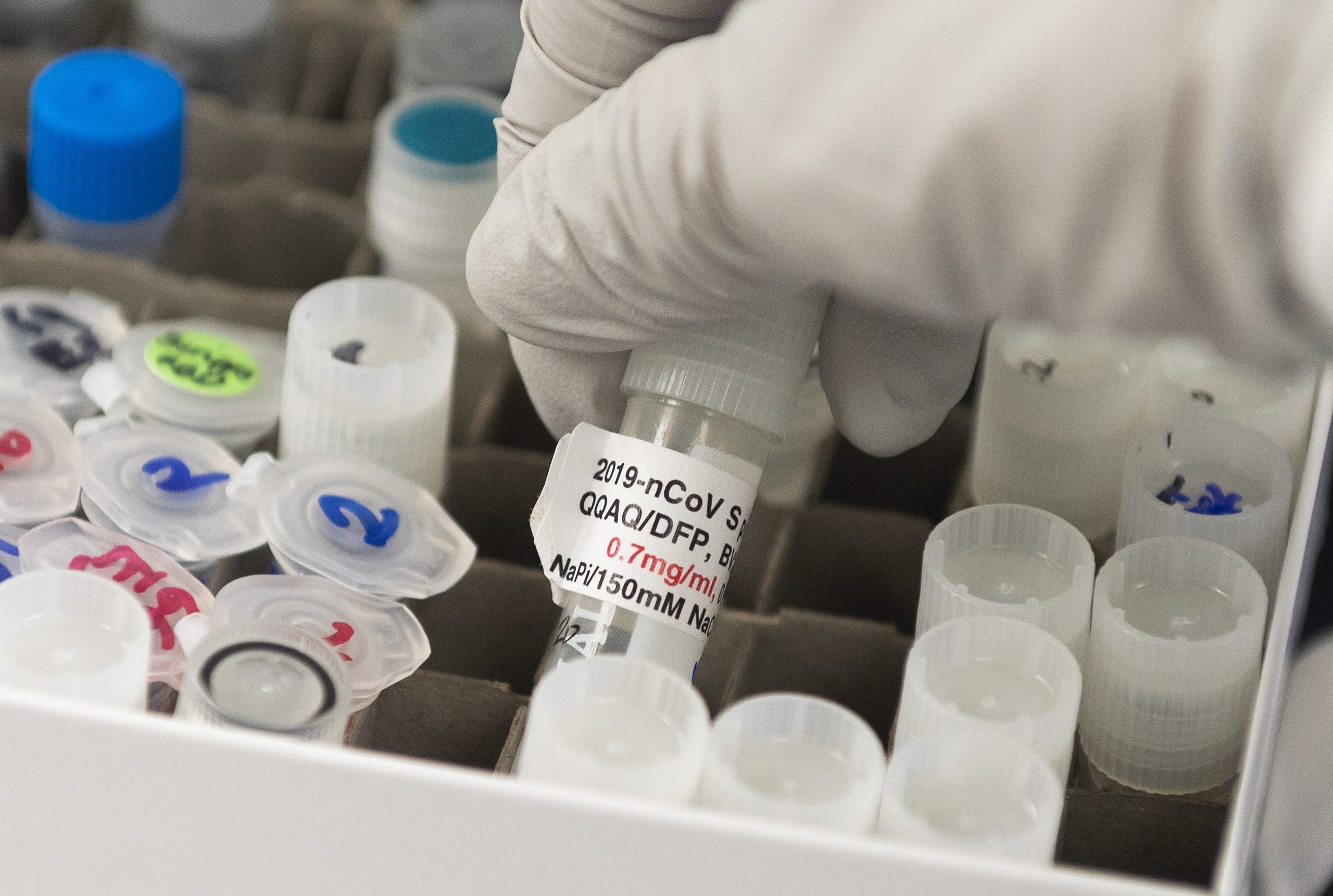
Billions of people are quarantined in their homes as governments try desperately to slow the progress of Covid-19, the disease caused by the Sars-CoV-2 coronavirus. With well over a million cases reported worldwide, health services in all countries are struggling to care for those who become seriously ill. A vaccine would save many millions from the disease, but we don’t have one, and it’s unlikely anything useful will appear for a year or more.
Vaccines work by triggering our immune systems to produce antibodies — proteins that bind to specific microbes and disrupt their biological processes or allow the immune system to destroy them, preventing them from causing disease. We have excellent vaccines against many viral diseases, including measles, mumps and German measles (or rubella) in the well known, safe and fantastically effective MMR vaccine. Once primed, the immune system retains a specific memory of previous infections and can obliterate returning microbes if they enter our bodies again. Vaccines safely mimic real infections, which also trigger antibody production and other immunological responses that provide immunity against future encounters with specific microbes.
Antibodies are currently central to many of our efforts to combat Covid-19. For example, antibodies harvested from previously infected people who have now recovered may offer a way to treat the disease. Recent Chinese data showed that five seriously ill patients, all on ventilators, had their viral load dramatically reduced when given serum containing antibodies from such previously infected people. All five patients recovered. The US Food and Drug Administration is now allowing American physicians to take a similar approach with serum from cured Covid-19 patients.
Antibodies are also the basis of the tests being developed to determine who has already had the Sars-CoV-2 infection. Without a vaccine, our current best hope of reviving the economy and getting people back to work is to confirm who has overcome the virus and developed antibodies against reinfection. But this strategy depends on the assumption that, once cured, individuals will have long-lasting immunity. Unfortunately, we don’t know if this will be the case.
It is certainly likely that people who have had the disease and recovered will have some degree of protection. A small study in monkeys found that recovery following initial infection prevented reinfection by a second exposure to the virus. However, these scientists could not study how long the immunity might last, although ongoing studies should provide more data on this. Different pathogens stimulate varying levels of immunity. As the first cases of Covid-19 were only formally recognised in China in January, there hasn’t been time to establish how long the antibodies the body produces in response to Sars-CoV-2 remain in circulation.
Reports of patients becoming infected a second time exist, but they are rare. A Japanese tour-bus guide suffered a second bout three weeks after having been discharged with a negative test result following a primary infection in late January. Whether she’d actually been reinfected as opposed to experiencing a relapse, or whether the test was wrong, has not been established.
Other viral diseases, such as flu, can infect us more than once, which is why we need repeat vaccinations. The flu virus can actually change the antigens recognised by the immune system in ways that make the antibodies made against one strain useless against the next. Fortunately, coronaviruses don’t, so far as we know, engage in this process of “antigenic shift”.
For most viral diseases, the immunity developed during recovery is robust, and this gives scientists hope that the risk of reinfection by Sars-CoV-2 is low. Recovery from yellow fever, for example, can trigger immunity that lasts a lifetime. Most of us benefit from the long-lasting protection gained from a childhood bout of chickenpox. The original Sars outbreak in 2003, involving a related coronavirus, also induced fairly robust immunity: antibodies to the virus were visible for three years or more after recovery. The same is true for the Middle Eastern respiratory syndrome (Mers) coronavirus.
However, some other coronaviruses that infect humans, such as those causing common colds, generally produce relatively weak immunological responses. Antibody levels wane after just a few months. Recent data produced by the UK Flu Watch cohort study, which constantly monitors for the appearance of different respiratory viruses in a group of volunteers across the UK, showed that reinfection by coronavirus types that cause common colds was indeed possible. However, the rate at which this occurs isn’t clear and some degree of immunity was the norm.
For Sars-CoV-2, only long-term data collection will tell us. However, the mathematical models used to predict where things are heading can examine scenarios where differing degrees of immunity are provoked.
Central to mathematical models is the reproductive number R0 (R nought), which reflects the number of additional people an infected person will go on to infect. For Sars-CoV-2, an R0 of around 3 means that every individual infected will, on average, transmit to three others. A simple calculation then tells us that when around 66 per cent of the population has been infected, the virus finds it increasingly difficult to find non-immune people in which to set up a new infection, and transmission declines.
This is the much-discussed “herd immunity”, in which a population builds up sufficient immunity to stop transmission. But it, too, depends on how robust our immune responses are, and how long they last. As the government in Wuhan in China, the original epicentre of the pandemic, is now tentatively sending its citizens back on to the streets, we will again learn from what happens there. Hopefully, this time, our government’s policies will be guided immediately by the findings.
Given how widespread Sars-CoV-2 is, Covid-19 will probably become endemic even if herd immunity is achieved. It will find enough new victims to maintain a transmission cycle, without spreading as we’ve seen during this breakneck pandemic. In this instance, regular exposure to the virus, even in people whose immunity is waning, will continuously restimulate antibody production. I consider it likely that the virus will stay with us, and remain a nuisance, but not the fast-spreading mass killer we see today.





