I The Man
For a moment, the world is as it used to be – unconfined, uncurtailed, alive with human teeming: coronavirus-free. The early light of a mid-April morning is already at the window. Sun-shot images flit through his mind: he’s playing somewhere in a rock pool by the sea with his two children; his wife is laughing. Then the half dreams fade and, already, he can sense anxiety seeping through some defensive wall in the back of his mind, pooling and mingling with the rising self-doubt. This is the peak, they say: today, tomorrow, soon.
Normally – the word seems to have to stretch itself further and further back in time – normally, Jim Down would kiss his wife and get up and head into work. But today he’s on the night shift at the hospital so he has to stay in bed, stop his mind racing, try to sleep. He needs to rest. The shifts have gone up from nine hours to 12. And they are relentless. How many days has he been doing this? He’s lost count. The world of medicine – his world, our world, the only world – has never been like this. There is no relevant history, no textbooks and no studies. Nothing is peer-reviewed or follow-the-procedure. The virus is obscure, monolithic, alien. They are fighting blind. Hand to hand. Bed to bed. He tries to sleep. But there’s a voice from his dreams that persists in his waking: Jo’s voice. “Are you sure,” Jo asks? “Will it be OK? Are you sure?” But he’s not sure. And so what is he going to say to Jo?
Jim Down is 49. He is slim, fit, fair and 6ft 1in with dark blue inkwell eyes in which other people write their stories while he listens – patiently. He has disconcertingly boyish looks and an old-school English demeanour – that odd mixture of determination and diffidence, confidence and anxiety, can-do courage and better-safe-than-sorry. He looks like the kind of man that Roger Bannister might have asked to set pace for him when he ran the sub-four-minute mile: two metronomically dependable laps without detectable fuss or falter before quietly standing aside to clap the other man home.
He’s also the doctor that you might have seen on the BBC evening news a few times. The first time in 2006 when he came out to announce the death of Alexander Litvinenko after the defector’s polonium poisoning by Russian spies. The second time on the main segment of the evening news on 6 April when Fergus Walsh, the BBC’s health correspondent – suited-up in plastic, visor and gloves – was briefly allowed to enter the Covid-19 wards of University College Hospital (UCH) in London. Jim’s voice is muffled behind the mask and visor but the whole country heard it cracking when he spoke: “I think it’s very hard on the families,” he said, “my kids are at home, my wife is home schooling. It’s easy for me, I’ve got a job and I am busy all day. They don’t really know what it’s like here – whether we are bringing home the virus – and they’ve been amazing. They just let me do what I need to do and I’m just incredibly grateful to them.”

Boyish looks and an old-school English demeanour: Jim Down, 49, is one of the consultants in charge of critical care at London’s University College Hospital. Credit: Kalpesh Lathigra
Jim’s wife is the actress, Patricia Potter. Coincidentally, she played a doctor, Diane Lloyd, in the BBC series Holby City. They were married in 2007. And the twins were born in 2009 – a boy and a girl.
Jim’s father was a doctor. His father’s father was a doctor. His mother’s father was a doctor. His own training began 33 years ago when he was 16 and he chose the A-levels that would lead to his studying medicine. Then five years at Bristol University medical school. Then a year as a house doctor, intern junior; qualified but unregistered. Then a couple of years in Exeter training as an anaesthetist. Until, finally, he came to London to start his real apprenticeship: seven truly intense years of dual training in anaesthetics and intensive care. He chose the former because it is a highly sensitive minute-by-minute discipline and then took the unusual step of adding intensive care because it seemed to him to be the extreme end of all disease processes. Now, he is one of the consultants in charge of critical care – the Intensive Care Unit (ICU) – at the pre-eminent University College Hospital in central London.
[See also: The wounded healer: How my father’s cancer led me to a life of helping others]
Tonight, that will mean he will lead as many as 75 hospital staff through the toughest night of their professional lives. He’s not sure of the number of patients yet but the count is rising. The expectation is somewhere between 60 and 80 – depending on admissions, on deaths. He strongly resists the idea that his whole life has been in preparation for this moment. Instead, he insists he is just a doctor doing his job surrounded by some truly exceptional colleagues. Everything is collaborative. He’s not a leader, let alone a hero. He dislikes even the word. He would much rather talk about the people he has been working alongside – how he’s witnessed them rising to the challenges and working in conditions unlike anything they have previously known. He lists fellow doctors and nurses and porters and physios and pharmacists and ward clerks until he is forced to move on. He doesn’t want to be formally interviewed, he says, and he doesn’t want to be quoted. All he wants is to let the general public know what that night in April – the peak – was really like for the health workers who dealt with it. Medically, psychologically, from the inside. Because little has changed, he says, and right now they are preparing for a second surge this winter.
The truth is that Jim Down is one of the doctors with the most hands-on experience of Covid-19 in the country. He won’t allow superlatives. But if you fell ill with the disease and you could ask for anyone, then you could do no better than ask for Jim.
Today, though, too-early awake, all he wants to do is get up and help home school his children, play with them, make their breakfast, talk. The weather has been unseasonably warm and it’s going to be another beautiful day. Good Friday. He wishes he was religious. But he knows only too well that it takes more than three days to bring people back from the dead. And that nobody rises alone. Each of the patients he sees in the ICU will have two dozen of the very best healthcare professionals looking after them at one time or another – all day and all night. A constant vigil. Every minute. Often for weeks.
The peak is coming. He shuts his eyes and tries to slip the knots of consciousness. In his half-sleep, he hears the sound of coughing and the wheeze of the machines. The peak, the trough, the test.
II The hospital
University College Hospital is a teaching hospital founded in 1834 in the north of the centre of London – near Euston station. Jim loves the place in the way a teacher loves the school at which they gave of their best – not just the buildings, but the atmosphere, the rooms, the rituals, the canteens, the meetings, the people. He drives into work because he lost the key to his bike on the first day of wearing the PPE – personal protective equipment; putting the gear on is easy enough but taking it off when every surface carries potential infection is an awkward and elaborate unpeeling fraught with layers of anxiety. An anxiety that attacks the quintessence of being human – touching, breathing, embracing.
London looks at its most attractive in the lower angle of the evening light. He has noticed that everywhere the cherry trees are blooming more intensely than ever – ivory, pink and pale rose – as if in urgent counterpoint to all the sickness. Like the birdsong. Like the weather. But crossing the city seems surreal. Everything is familiar; everything is unfamiliar. The dissonance between the emptiness of the streets and the hitherto routine footfall of millions affects him in ways he cannot process. Likewise, listening to the news as he drives is almost hallucinatory. Not the details of the broadcast – which often seem distant and irrelevant compared to the intimate reality of his daily combat with Covid-19 – but the astonishing fact that every guest and every item on the show is focused entirely on his job. There’s nothing else. And it’s the same on every single news programme – it’s all about medicine, the virus, the lives saved, the lives lost; the work he and his colleagues are doing. And it sounds as mad and dystopian to him as it does to everyone else.
He catches the government minister saying they are expecting the peak to be over soon with a note of – what? – enthusiasm in his voice. He listens with ears precisely cognisant of the truth. The truth that they were too slow to lockdown; that the government had due warning but was sluggish and facetiously contrarian; that preparation was poor; that weeks were lost; that lives were lost; that some of the other hospitals have already fallen over and sent their patients to UCH; that many are woefully short of the protective equipment they need. He turns the radio off. He has noticed that these wider truths become more and more irrelevant the closer he gets to the hospital itself. The objective becomes subjective each time he steps over the threshold. The numbers become names. He ceases to care about the politics, the statistics, the arguments and to care instead for the patient in front of him. Over at St Thomas’ Hospital, one of the other great London teaching hospitals, the patient in front of his opposite number this weekend is the Prime Minister.

Holding on: Jim Down by the oldest part of University College Hospital, a place he “loves… not just the buildings, but the atmosphere, the rituals”. Credit: Kalpesh Lathigra
He parks in the space donated by a member of the public and walks towards the hospital. He thinks about the calls he has to make. Jo and her husband, David, have somehow got to him. He knows what it is: it’s the way Jo asks the question, “Are you sure?” Not in a nasty or even passive-aggressive way; but because this seems a reasonable question to ask a doctor. But the problem is nobody knows anything about the disease. The problem is that nobody is sure.
On Tottenham Court Road, he feels another surge of anxiety. He wonders if he should go to live in a nearby hotel to protect his family at least. He knows for certain of nine fellow staff members who have the virus; he was sat in airless rooms with them for weeks. There is fear circulating. He’s never experienced the medical community like this. The rumour mill – yes; but, also, the daily reporting of the actual deaths of fellow doctors and nurses and health workers. And they see every age and every type of person with Covid-19. A 29-year-old died two weeks previously – no underlying health issues. He has read some journalism that is cavalier and fatuous and he is concerned that the wider public has not grasped how terrifying this illness becomes. Of all the deaths he has seen in the ICU, these are the worst. The struggle for breath. The sudden inexplicable deteriorations. No loved ones present. Too many people are dying face down and alone surrounded by the muffled murmur of strangers dressed in visors and plastic.
He treats his anxiety by hurrying inside the hospital. Peak or no peak: they will all do their best for each and every patient. And, once inside, he feels the instant relief of purpose, work and focused colleagues. Something truly remarkable has happened at UCH. Something life-affirming in its way. A complete and serious transformation at incredible speed. They are as ready as they will ever be. He heads towards the lifts. For the first time since he awoke this morning, he feels pride and resolve flooding back.
They knew what was coming. One of UCH’s top professors – Mervyn Singer – called European friends and colleagues in Italy back in February and early March. Their chief executive Marcel Levi – who is also a professor and front-line clinician, born in Holland – had spent a long time working in Perugia. So the community of European doctors communed and medical staff learned everything there was to know first-hand and in as much detail as their fellow professionals could give. The lackadaisical UK government seemed to be ignoring the advice so the medics ignored the government. By early March, all the senior staff were coming in additionally on their Saturday nights to go through plans, protocols and detailed preparation.
They got as far ahead as they could. They ensured they had the equipment they would need – and, crucially, lots of oxygen. They converted eight out of the 12 operating theatres into Covid-19 wards. They changed a stroke unit into a 28-bed high dependency ward – solely for Covid-19 patients. They had their normal ICU units optimised for Covid-19 to deal with whatever the peak turned out to be.
Meanwhile, 35 consultant anaesthetists became intensivists – adding to the normal 18. Seventy or so doctors from all over the hospital were enlisted to help – surgeons, gynaecologists, dentists, urologists, paediatricians, trainees and neurosurgeons. They went from 180 nurses to nearly 350. From nine physios to 45. Five intensivists came over from Great Ormond Street along with ten specialist intensive care nurses.
Jim’s pass bleeps him into the ward. Tonight, he thinks, UCH is totally focused. If you trained for anything in medicine, then tonight you trained for Covid-19. Apart from babies being born, this hospital is doing nothing else.
III The Intensive Care Unit
He goes into the consultants’ office. This is the handover. Normally (that word again), he would be being briefed by one person about maybe 15 patients, but now there are four consultants briefing him on just short of 70 patients – all with Covid-19. He will be the sole lead on the night shift. The smaller London hospitals are sending more patients – struggling for PPE equipment; not enough oxygen; no capacity. The other doctors – his friends – highlight two cases they have that they think need his immediate attention. He’s struck afresh by their calm, their rigour. The challenge is that all the patients need immediate attention. Continually. Everywhere, in every bed, life is held tenuously. He goes to put on his PPE as fast as he safely can.
He is careful to remain outwardly assured but he walks at double speed on the ward. He takes one look at the two patients – Andrew and Beth – and he makes the decision: they both need to come down to the ICU. This is the first of roughly 200 decisions he will make on the shift tonight. They are both in CPAP (Continuous Positive Airway Pressure) oxygen masks and there are serious risks with moving them – if anything goes wrong in the lifts, where there is no life support, they will die. But they have to be taken down. They need to be intubated – the inserting of a tube down the trachea so that a ventilator supplies oxygen to the patient directly to the lungs.
He lets his eyes travel around his assembled colleagues. They all know the same thing: that Beth is a nurse and that she was working in a Covid-19 hospital, as they are all doing now. He says he will lead Beth’s intubation himself.

Keeping vigil: intensive care nurses prepared to care for patients with Covid-19. Credit: Christopher Furlong/Getty
Now the night starts to move at speed. He makes his way through the wards. The beds come at him. Curtain after curtain. Patient after patient. So many so seriously sick. He is grateful to be surrounded by so much competence. He confers with his colleagues as he goes – trying to hear and be heard through his visor without raising his voice. If he were to never stop, eat, go to the toilet, or do anything else, he would have roughly ten minutes per patient. He has to go faster than he has ever gone before. He has to go slower than he has ever gone before.
At every bed, he checks the date of the patient’s symptoms. The date of intubation. Are they on antibiotics? Should they be? Is there a secondary bacterial infection with which antibiotics might help? Or is this just what Covid-19 looks like? In which case – will the antibiotics be useless and even harmful? And which antibiotics? Or could there be a secondary fungal infection? Nobody knows the answers to any of these questions.
Should he thin the blood? There’s lots of talk about high rates of blood clots forming in the legs and breaking off to the lungs – but what about the risks of bleeding, especially in the brain? Is the ventilator set optimally? Should he lighten the sedation and allow them to “breathe up” and interact with the ventilator or will that perpetuate the inflammation and make things worse? Or should he keep them deeply sedated and fully ventilated which means they’ll be so much weaker and delirious from all the sedatives – and is that worse? Nobody knows the answers to these questions either.
Should he give fluids to help the kidneys – or keep them dry to help the lungs? Why do so many get kidney failure? Should he give steroids? Why has this patient got worse all of a sudden? Why is this patient improving? Nobody in any hospital knows the answers to any of these questions. All they can do is learn fast and maintain total vigilance.
There are so many patients. Doctors eddy and mill around the beds. He thinks: the nurses are working at a level that no human being can sustain. He thinks: this is what courage looks like – raw and unmediated.
Already, 60 minutes in, the PPE equipment has become nightmarish to work inside: hot, claustrophobic, disorientating and alienating. He can feel – physically feel – the strain that everyone is under. They all have to put their names and their roles on their chests because they can’t recognise one another. Everyone suffers from the crushing headaches. Inside the visors, they can no longer hear one another clearly above the whirr and beep of the life-support machines, the alarms, the dialysis pumps, the computers, the treatment systems, the air conditioners.
Normally, they pop in and out of the bays, passing on medical or patient information; but instead, every conversation has become cumbersome and strained. They have to use walkie-talkies to communicate with fellow staff outside the ward every time they need something, because they can’t take the PPE off and then put it back on. And they are tearing through supplies.
[See also: The young doctor’s dilemma]
The psychology is – if anything – worse. Normally, the ICU would be a balancing act between those recovering from elective surgery and those arriving from Accident and Emergency. Normally, he’d be doing a nine-hour shift with a group of people – all of whom he knew and who knew each other. Normally, the unit would comprise patients who have the full scope of acute conditions: pancreatitis, accident trauma, meningitis, sepsis, brain haemorrhages, drug over- doses, suicide attempts. Normally, there would be a whole history of medicine and experience to deal with each and every one. Normally, there’s a route to recovery.
But not now. Now, everyone is ill with the same new disease. And there’s no cure. This is as crushing mentally as the PPE is claustrophobic physically. Bed after bed of immobile human beings lying faceless on their fronts. Machines keeping them alive. This is the vision of the virus. Like something too dark even for Philip K Dick or William Blake. He tells himself again to remember to recognise that none of the people are working in their normal environment or doing their normal job.
There is something, too, about the fact that Covid-19 is in the atmosphere, in the very air, that makes it worse. Even as they work, the staff are all dealing with the fear of actually dying themselves. And this is not a vague fear such as the public might suffer; but a fear born of watching their fellow professionals being wheeled in – here, now – because here comes stricken Beth, the nurse, through the ward.
At least she has made it down, he thinks.
IV The Procedure
The medical staff gather at Beth’s bed. Jim Down lets his eyes go round his colleagues again. There is a surgeon doing a junior’s job. Two more doctors who did not choose a career in intensive care. An ICU nurse. A dental surgeon. A nurse who was brought in from paediatrics at short notice. His fellow anaesthetist, Mike. They all wear the stress differently. In the last few days, he has witnessed every human reaction – from tears and breakdown all the way through to the counterproductive fortitude of staff who refuse to rest. Now though, he can sense the unease somehow coming through the plastic gowns they’re all wearing. He checks the monitors. Even in normal times, intubation is a serious procedure. With Covid-19, it becomes much, much more difficult.
Normally, he would hold a mask over the patient and give them roughly three litres of pure oxygen into the lungs. This would buy him some time. The oxygen saturated in the patient’s blood would stay at a good level – hopefully above 90 per cent – for maybe five minutes simply by using the three litres they had already inhaled. He would then put the drugs in. Put the patient to sleep. Paralyse them. All the time, he would watch the readings of the oxygen saturation in the blood – the “sats” level as they call it. He would insert the tube past the vocal cords and into the trachea. Any drop in the patient’s levels of oxygen in the blood would come back up to 97 per cent – optimum – as soon as he had got the tube in.
But the problem is that Covid-19 patients are already on pure oxygen from the mask; he cannot turn it up any higher. Beth has all the oxygen possible; he can’t get any more into her lungs. Worse, when they take Beth’s mask off, he knows that she will immediately start to turn blue. Covid-19 patients cannot last more than a minute without full oxygen support. The oxygen in her blood will immediately start to drop. And when it hits 90 per cent, it begins to drop even faster, the rate of descent accelerating. The whole procedure, therefore, which would normally take five minutes, has to be done in less than one.
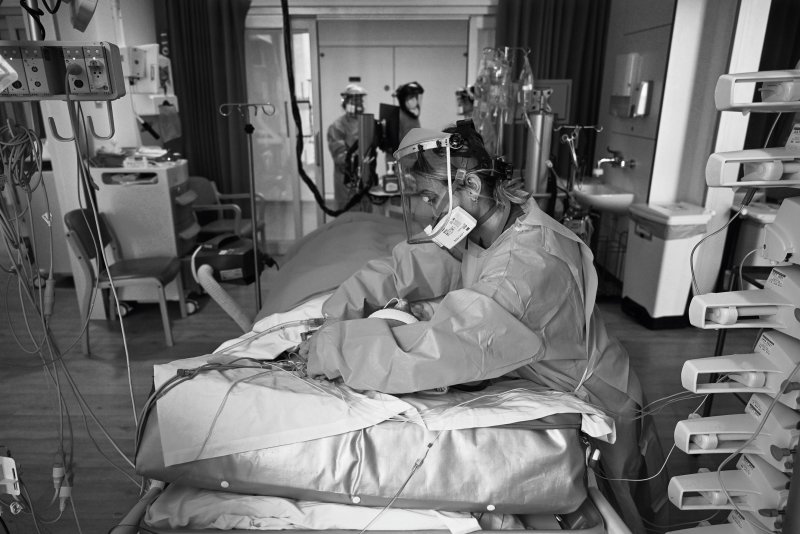
Critical condition: a hospital intensive care unit. Credit: Neil Hall/EPA/Bloomberg
He is the team leader. He needs to keep the atmosphere calm. He has done this operation himself many times but it’s important that there are as many anaesthetists as possible capable of doing it in the time. And Mike is one of the best.
He checks everyone is ready and gives the signal. The pressure is intense. All the alarms go off immediately. Beth’s blood oxygen saturation level drops – 80 per cent, 75 per cent. Mike has the metal blade over her tongue so that he can access the trachea. But, involuntarily, Beth is coughing. Aerosol Covid-19 straight onto Mike’s visor. Outwardly, Jim is still calm. Sats at 65, he says, quietly. But inside, he is screaming – get on with it, get on with it, get the tube in. Every moment could be a catastrophe. Mike’s hands are steady. Jim watches him manoeuvre the tube – delicately, deftly – with total concentration and precision. Sats at 55 per cent, he says. They don’t have the option to abort because this is Covid-19 and Beth won’t make it back on the mask. They have less than ten seconds before her heart stops. Mike gets the tube in. Jim hooks up the machine. She’s at 50 per cent. But they’re in.
Normally, the sats would now climb but, this being Covid-19, the oxygen in Beth’s blood is rising far too slowly. Jim thanks Mike and gives the immediate instruction for the team to get her on her front. The back of the lungs are usually more inflamed with the disease; the front are usually in very slightly better shape. He can see one of the doctors blinking back sweat – resisting the overwhelming temptation to wipe his eyes. He thinks that despite all the organ and blood support it comes down to something very basic: on her front, Beth might live: on her back, she will die.
The team goes into the preparation. Each time they turn patients, it is difficult and dangerous. There are all the airway tubes. There are the lines in for all the drug infusions into the neck. There are the lines into the arteries. There’s the catheter. The dialysis lines. They lose or twist anything and Beth will crash. And, of course, Beth is unconscious so the risk of injury is increased. Are her eyes covered and protected? Is she ready? Yes. They look at one another through their visors. Ready, steady, he says as loud as he can. And turn.
Beth is on her front. The oxygen begins to crawl back up. He checks his watch – he’s running late. He has to get out and call patients’ relatives. He can’t keep them waiting. For each of them, Jim Down knows, his call is vital, their lifeline.
V The Relatives
Normally, the relatives would be here, of course, and he’d speak to them in person. Normally, they’d be sat around the beds bringing all manner of gifts; doing what human beings do in love and solidarity to cheer and comfort one another. But now they are in a particular state of absent agony: unable to visit, unable even to speak to their fathers and mothers, sons and daughters. Cut off. Anxious. Locked down at home and listening to the death count climb every afternoon.
He takes off his PPE – slowly, quickly – and walks to the nurses’ station where the phones are set up. There is a team of volunteer hospital staff who field all the calls. They make lists of relatives. They check everyone has been called back. They help with the video calls. Their work is tireless and means everything to the relatives ringing in. He is chary of the phrase “unsung heroes” – but in any case, he says, there are not choirs enough in Britain. They give him the numbers. He wishes the hospital had time to find an area a little less public for these conversations. But nothing is ideal and all he can do is lean away from the other staff and into the receiver.
Normally, one of these calls would be a psychological ordeal for any doctor. Jim Down is experienced, of course, but there’s nothing that really prepares you for talking to someone about how close to death their mother is, their father, their son, daughter, sister, brother. Tonight he has four calls to make. Three now. One later. He is relieved the call to Jo will be in the morning – at around 6am – after he has again checked on David. He takes a breath. He is pleased at least to be out of the PPE. He makes a conscious effort to take account of how important each word he says is to the person with whom he will speak. Each call has to take as long as it takes. But he has no time. More patients are being admitted. And he’s needed urgently in the theatre as soon as he can get back there.
He picks up the phone and listens to a daughter crying for her mother. She wants so badly to come in to see her mum, she doesn’t care if she gets it. The second call is overseas. He can hear the agony in the son’s voice – the self-recriminations: he should have flown back at Christmas, but he didn’t know, he didn’t know. On the third call, he has to tell a young woman that her dad is deteriorating; that the prognosis is not good; that at 77 it is likely that the machines are torturing her father; that the route back is very hard now. He has to be honest – he says that there’s only a very small chance that her dad will make it. She asks him what he can do? Is there anything – anything in the world – that can save her dad? He can’t think of any way to answer her question except with a promise: I’ll do everything, he says, that I would do for my own dad.
VI The Virus
Sometime in the dead of the night, Jim Down is on his way towards theatre where there are three patients in urgent need of his attention simultaneously. It must be 2am or 3am. These are the hours where the night seems both to shrink and to stretch and to open before him like a void or a black passageway leading deeper into absence – or darkness, he’s not sure.
He thinks about the virus as he walks. There are WhatsApp messages all the time from the international medical community, research papers shared, but it’s too soon for meaningful data. He reads what he can whenever he can – lifts, queues, awake when he should be asleep – and he is moved by a sense of the collective: human beings everywhere questing for the same information all over the world. Science, medicine, the effort to understand the workings of reality. Everything else comes second now: art, sport, economics; the posturing of politicians; the phoney proclamations of religion. Something has been proven, he thinks, something profound in the communal psychology about where we place our true reliance. Perhaps the clapping is a sign of this. What he and his colleagues would like most of all, though, is proper funding and a trustworthy government.
The virus. Most people he sees have had the fever – a three- to four-day illness – and then a sickening second bout around day six or seven. This is where they start to worsen – nobody knows why some and not others. Genetics? Their body’s inflammatory response? In any case, the breathlessness has usually become acute by the time they are in front of him and their tissues are starting to be deprived of oxygen: hypoxia. On the chest X-rays, there are infiltrates – the typical shadowing of both lungs that looks somehow medieval, he always thinks, like they’re fighting something they don’t understand. Which they are and which they don’t.
There are often the classic blood signs: a drop in lymphocytes, the white blood cells involved in the protection against disease; and all the markers of inflammation are up. Some people come back after being on CPAP, rally, recover. Others struggle. When they have to intubate, they attempt to ventilate the lungs gently – it has to be precise, careful. Human lungs are highly sensitive. Too hard and the inflammation gets worse. They dialyse the kidneys. The machines take over. Sometimes the inflammation settles down. Sometimes the blood markers settle. Sometimes the patient starts the long and difficult journey back.
But, sometimes, the oxygen levels stay stubbornly low. Patients fall into acute respiratory distress syndrome. And now mechanical ventilation becomes even more difficult as the machine tries to get oxygen in without injuring the lungs or causing abnormal pockets of air to form between the lung and chest wall. The lungs become fibrotic – stiffer – and it becomes harder to get the carbon dioxide out. The patient dies slowly of hypoxia.
He passes bay after bay. The hospital is at full stretch. He has never seen a night so busy. As he’s crossing the walkway between buildings in the hospital, he catches sight of the night sky. All week, a huge and sickly pale moon has been lumbering across the heavens – as full and as close as it ever comes to the Earth. The super-moon, they say. The perigee. The peak. Easter 2020. His fervent hope is that this time will come to be known as the worst few days of the virus in the United Kingdom. They need to keep the numbers down. There is no other medicine possible in these conditions. If the infection rate climbs, then you risk lives and you shut down the hospitals for all the other emergencies. Many people die. Simple as that.
He enters the last bay in the converted operating theatre and pulls back the curtain. He stands a moment in the semi-darkness. The very air seems crushed in here, as if the night itself is struggling to breathe. Life has shrunk and shrivelled to almost nothing – the heaving of machines. He has the momentary feeling that this is the very centre of the disease; the inner chamber where the virus sits enthroned, preening and sneering, malign, intelligent.

Faith in the time of coronavirus: a hospital prayer room displays social distancing guidelines. Credit: Getty Images
The nurse, Maria, is alone. Through his visor he can see the stretched contours of her face. From her body language, he intuits that something is seriously wrong. She is one of the very best he has ever worked alongside – buoyant, funny, rebarbative and resilient beyond any measure the hospital has yet conjured. They have laughed together, worked together, dealt with all manner of triumph and tragedy, life and death. She gives better than she gets. She’s a leader and an example and would consider herself neither. She is the nurse he would choose to look after his own children.
She’s been here all night. He stands beside her. She would normally have said something by now. She is checking lines in. Working at three times her usual speed. He asks about adding some enoximone, another infusion for the heart. But something is wrong. And when she looks at him again, he can see what it is: she is furious. Her eyes are narrow and molten hot with fierce accusation. She stands back from the patients and rounds on him.
I cannot do this, she says. I cannot do this for five patients at the same time. You need to sort something out, Jim, because this isn’t working.
[See also: Personal story: On the Covid frontline]
He stands still and listens. Keeps his eyes steady. Nods. He’s screwed up. He’s come marching in and merely added to her workload. The nurses cannot do any more. His heart goes out to her. He has never seen her like this. The truth is that the people who watch the patients are the nurses. Hour after hour into the night – an unceasing vigil – all the time, acutely hypersensitive to every change, imagined or otherwise. Yes, he thinks, the public should know: it is the nurses who truly contend with this disease – close up and physically, with their hands and with their eyes.
Normally, Maria would have one patient to care for. Normally, she would have one night-plan per patient to administer. This means drawing up the drugs, giving the drugs (all of them dangerous), running complex machinery – the ventilators, the disposable parts of the dialysis machines, dealing with a whole host of infusions for sedation, monitoring blood pressure and heart output; managing the needs of feeding, bowels, urine, mouth care, eyes. But tonight Maria has five patients to care for and she’s trying to deliver a level of care to each and every one of them that would make her proud. Not even proud: just what is right. And that level of care is not possible.
There are other nurses who are willing to help but they’re not trained. You can’t become an expert in a week. ICU nurses are highly specialised and in very short supply. He is well aware that every hospital in London is desperate for them. That’s why all the new Nightingale wards worry him. You can build the beds. You can even get the equipment. But there are only so many doctors and nurses who are trained in intensive care. And so many of the nurses are from overseas and from the European Union. He wishes the nation could see what he sees. Why would a government seek to alienate its own nurses? What kind of men would knowingly turn a nation against so many of the people who care for its sick?
He feels a reciprocal charge of anger. The heat and claustrophobia in here are intense. OK, he says. You are completely right. We need a plan for now and we need a plan for how we’re going to relieve nurses of some of this work. Maria calms. Yes, she says. Yes.
Three out of the five patients are in trouble now. Not because of anything Maria has or hasn’t done but because everywhere tonight, patients are suddenly collapsing, because that’s how Covid-19 works. He makes another decision. Normally, they can do everything in parallel. But now they are going to have to work in sequence. Who first? Another decision. Frank first.
Frank is in the deepest trouble. Let’s simplify things, he says. Let’s simplify the heart drugs. Let’s go to adrenaline. Deal with that problem. Yes, Maria says. They pick up a walkie-talkie so they can order up what they need. Right – now let’s get the dialysis up and running. They work together. But as they do so, a junior arrives and tells him that Patti’s carbon dioxide is climbing behind them. He has to go over to Patti immediately. His mouth is dry. He needs water. He can’t use a stethoscope for fear of infections. He has to use his experience, do everything by feel, look at the ventilator. He changes the filter and alters the setting.
More alarms. The third patient is crashing – Louis. Alarms going crazy. He switches beds again. Everything is hard to assess with Louis because he is on his front. He scans all the equipment, his eyes like blisters. The virus is here in the room – a presence. He can feel it. In the air. In the throats of the patients. On their PPE. Maria is beside him. There are no more ICU nurses free and there are no more ICU consultants. Everything that happens now happens because he and Maria manage it. Life or death again.
Ten minutes later, he’s greatly relieved to be joined by one of his anaesthetic consultant colleagues. More nurses arrive. Another doctor. They all work together. Deep in the physical lives of their patients: their throats, their kidneys, their lungs, their hearts, their blood, their excretions, fighting the virus, moment by moment, alarm by alarm, staving off death as it comes at them again and again, now here, now there. This is the true meaning of the peak.
They stabilise all three in turn. He hates having to choose but this time it has been OK. He stands back. For a second, his mind travels from the asphyxiating crucible of this operating theatre and he thinks about how far human beings have come – through all of human history until now. And here they stand: half a dozen men and women in semi-darkness, swathed in blue plastic, blue gloves on their hands, masks, visors, surrounded by more human beings who lie all-but-dead on beds around them – tubes into their lungs and veins and organs. Here they stand, working to sustain life itself, which is the only miracle he truly believes in. When it comes right down to it, there is no greater sanctity than life, and no greater religion than reality. He looks up and tries to convey some warmth of fellow feeling merely through the movement of his eyes.
Maria smiles back. We’re going to get these bastards back to their families alive, she says, and they can bloody well take care of them.
VII This is Jim Down
The sun is rising. Easter Saturday. Someone comes over and says that the nurses have got a tablet to David, Jo’s husband – and would he mind doing the call back on the ward all together? He had forgotten about Jo. The emergencies have been relentless. But this is good news, he thinks, because it might be easier if David is on the call so that Jo can see and hear her husband’s condition for herself. He’s made the decision to intubate David. He can’t delay any longer. He had been dreading telling Jo this on the phone – all her questions that he could not answer.
Perhaps it’s the night, perhaps it’s because he is roughly Jim’s age, perhaps it’s because Jo is roughly his wife’s age, perhaps it’s because David and Jo also have two children the same age as his own, but Jim is affected as soon as he arrives at David’s bed. The nurses have put a tablet in a clear freezer-storage bag and David is struggling to talk to his wife, Jo, on the screen through the smothering effect of the plastic and in between desperate gasps from the CPAP mask.
What affects Jim is not just what David is saying but also the way that he is saying it. Only around 50 per cent of patients who are intubated survive, and David somehow knows this. Jim can tell that David is therefore trying to say that he loves his wife without upsetting her – without sounding like he thinks he’s going to die. He’s trying to say his last words without them sounding like his last words.
“You know that I love you.” David’s voice is hoarse, his breath perilously short. “You have everything you need to be OK. You know that I love you. You know that I love you. Tell the children I love them every single day. Promise me. Tell them every day.”
“I love you, too, David,” Jo replies. And Jim can tell that she is valiantly trying to give her husband courage and reassurance in return – also without sounding as though she, too, is afraid he’s going to die. “And when this is over,” she says, “we’re going to take the kids and show them where we got married. I love you so much, David. And I know you are going to get through this.”

Peak practice: “the hospital is at full stretch. He has never seen a night so busy”. Credit: Kalpesh Lathigra
Three things he has come to understand. Human beings are capable of breathtaking dignity. Human beings are capable of breathtaking compassion. And, in the face of death, all human beings want to hear and to say the same thing: “I love you.”
That’s all there was, or is, or could ever be to say. It makes no difference, of course, to the virus, to science, to the swollen moon or the rising sun. But it makes all the difference in the world to human beings.
“I love you very much David,” Jo says – she waves at the camera and now Jim can tell that it’s costing her everything she has not to cry. “You’re the love of my life.”
One of the nurses has turned away. Jim has forgotten for a moment that he is in charge of this man’s care. He forces himself to grip his own emotions and then leans forward so that he appears in the camera line and so that Jo can see him. And he says the only thing he can think of to say.
“Hello Jo, this is Jim Down. I am David’s doctor. We spoke on the phone. Don’t you worry: we’ll take good care of David. We’ll take very good care of him.”
With the exception of the main protagonist, the names have been changed in this piece.
[See also: A London NHS hospital chief reflects on the peak of Covid-19]
This article appears in the 27 May 2020 issue of the New Statesman, The peak






